“If only, he had access to his HIV treatment. If only, he could travel. If only, we had reached him in time.”
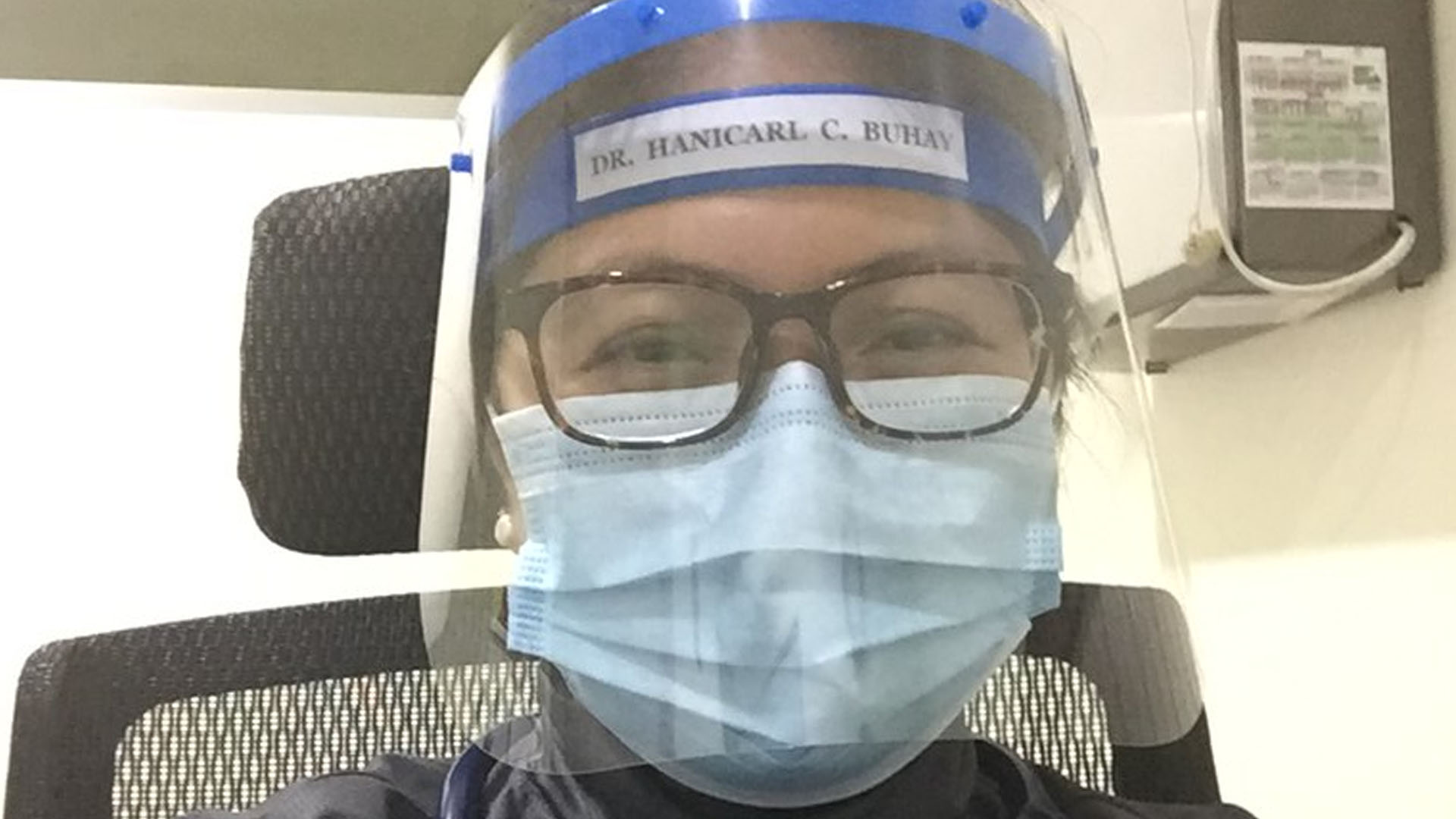
Dr. Hanicarl Buhay replays this “If Only” game in her mind as she recalls how the COVID-19 pandemic has significantly affected her patients with tuberculosis—resulting even in the death of a person living with HIV (PLHIV) who underwent TB preventive treatment (TPT). Buhay is a Medical III Officer who works at the TB clinic of the Batangas Medical Center.
“He was in his 40s when he got infected with HIV. He was referred to us by the hospital’s Wellness Clinic,” explains Buhay. According to the doctor, persons living with HIV are advised to have TPT to protect them from the TB bacteria.
“We were able to start him on his anti-TB medication but then the quarantine happened,” Buhay recounts. The patient at the time lived in Nasugbu, which was about two hours away from the hospital. Fortunately, when community lockdowns were enforced, Buhay was able to give him a month’s supply of his anti-TB medicines.
But despite measures to continuously administer treatment for TB, challenges in providing treatment for HIV complicated the patient’s path to recovery.
The doctor further remembers that it took a while before the patient resumed his HIV therapy because of lockdown protocols. By the time calls were made to have him transferred to Batangas Medical Center, his situation had worsened, and it was too late when he finally reached the hospital. Buhay and her staff were disheartened when they first heard news of the patient’s death.
“We have come to know him on a deeply personal level,” she says. She admits feeling awkward talking about a death when her family name literally means “life”.
During their initial consultations and visits, Buhay remembers how the patient was so determined to get well. She recalls encouraging him, “There’s nothing wrong with you for having HIV, you can still enjoy your life. You just have to take the medications and the therapy to avoid complications.”
“It was such an unfortunate time,” laments Dr. Buhay. “When you have patients who are so willing to undergo therapy and medications, but then to have these uncontrollable forces come along the way.”
More than medication
Dealing with TB patients, especially those diagnosed with HIV, Buhay explains that there is a lot of emotional care extended as well. Aside from administering medication, the process also involves therapy and counseling.
“We don’t only talk about medicines and treatment regimen. We also talk about their relationships, their plans, and life in general,” she says.
Looking back, Buhay understands that the unfortunate circumstances faced by her late patient can further serve as lessons to improve health services. She hopes to address the negative stigma surrounding TB and HIV patients and to also increase accessibility to treatment and facilities in rural hospitals.
Furthermore, Buhay believes it is important that tests should be done as soon as the earliest signs begin to show.
“TB is just like any illness that has its own treatment and medication. We should not discriminate the people with TB. It is so important to make treatment more accessible, especially during such difficult times where a lot of sectors are affected by the lockdowns,” stresses Buhay.
With an illness that requires strict compliance in administering medication, the slightest delay in treatment could lead to the most detrimental of results—a harsh reality that Buhay and her team knows too well.
Moving forward, however, she and her team have found a firmer resolve to overcome similar challenges that their many TB patients may be currently facing. With TB-diagnosed patients facing higher health risks during the current height of the pandemic, Buhay endeavors to ensure continuous treatment even amidst strict lockdown protocols, limited operations, and little to no travel.
Treating patients under lockdown
During her two years at Batangas MC, Dr. Buhay has efficiently handled all referrals from in-patients and out-patients. But it became a different scenario when lockdowns and strict quarantine measures were implemented in the country.
“We were also affected by the lockdown,” remembers Buhay. “But thankfully we are still able to continue our services up to this day while health protocols are still in place. We still maintained operations from 9-5, but in order to accommodate our patients, we gave them medication good for a month or a month and a half as long as they could follow compliance. We even set up a Facebook page where they can easily contact us and our staff.”
In curing patients with TB, Buhay stresses that adherence to treatment was critical to control the spread of infection. She was thankful that majority of patients continue to contact them despite the new situation. In return, their clinic strived to refer them to the nearest facility for continuous medication. Their clinic even coordinated with local health units to provide their patients with medication which their hospital is willing to pay and replace after the lockdown.
“As a doctor, nothing brings me more joy than seeing them recover,” shares Buhay. “But it really depends on the patient and their compliance to the medication. As they show their willingness to keep receiving treatment, it is within our duty to only guarantee that the medication is easily accessible to them.”
With the new normal in full swing, Buhay adapts the lessons she has learned as she continues to treat patients under lockdown. Despite the passing of one, she still look forward to the days where hospital visits with her patients would turn into joyful conversations and catch-up sessions on their recovery.
With a renewed vigor, Buhay tries very hard not to wallow in this “If-Only” mindset. Seemingly giving a nod to her own surname, she reflects: “Life is definitely worth living.”